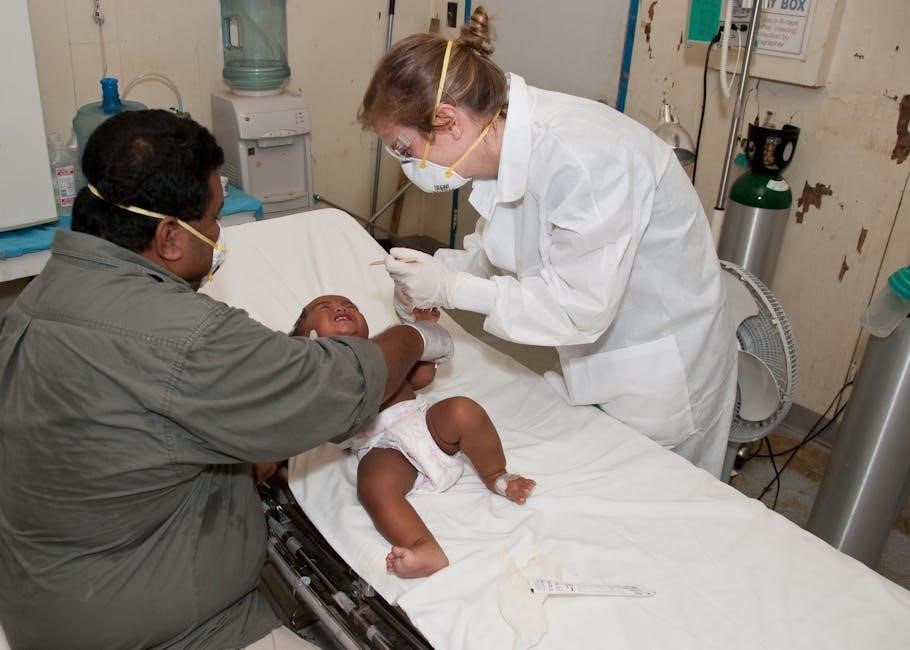
Pediatric Advanced Life Support (PALS) Overview
PALS training, often found as a PDF resource, equips providers to manage critically ill infants and children. Guidelines are regularly updated,
reflecting current resuscitation science and best practices from 2020-2024.
What is PALS?
PALS, or Pediatric Advanced Life Support, is a comprehensive, classroom-based course designed for healthcare professionals who may care for critically ill or injured children. It goes beyond basic life support, focusing on advanced resuscitation techniques tailored to the unique physiological needs of pediatric patients. A readily available PALS PDF manual serves as a crucial resource, detailing algorithms and protocols.
The course emphasizes a systematic approach to assessment, intervention, and teamwork. It covers topics like recognizing respiratory distress, managing cardiac arrest, and providing pharmacological interventions appropriate for children; The 2025 AHA/AAP guidelines, built upon evidence from 2020-2024, are integrated into the curriculum, ensuring providers are equipped with the most current knowledge. Mastering the PALS PDF content is essential for successful course completion and competent patient care.
Importance of PALS Certification
PALS certification is critically important for any healthcare provider potentially involved in pediatric emergencies. It demonstrates a commitment to providing the highest quality of care to young patients, equipping professionals with the skills to effectively manage life-threatening situations. Access to a detailed PALS PDF guide is invaluable for both initial learning and ongoing reference.
The course reinforces the importance of systematic assessment, early intervention, and effective teamwork – all vital components of successful pediatric resuscitation. Staying current with the 2025 AHA/AAP guidelines, as detailed in the PALS PDF, ensures adherence to evidence-based practices. Certification not only enhances individual competence but also contributes to improved patient outcomes and a safer healthcare environment for children.
The PALS Algorithm: A Step-by-Step Guide
PALS algorithms, often detailed in a comprehensive PDF, prioritize BLS, airway management, and pharmacological interventions for effective pediatric resuscitation and stabilization.
Initial Assessment & Recognition of Distress
Initial assessment, thoroughly outlined in PALS PDF resources, begins with evaluating the child’s appearance, work of breathing, and circulation. Rapidly determine the level of consciousness using the AVPU scale (Alert, Verbal, Painful, Unresponsive). Assess respiratory effort – noting rate, depth, and any signs of distress like nasal flaring or retractions.
Simultaneously, check the heart rate and peripheral perfusion, looking for capillary refill time and skin color. Recognizing early signs of deterioration is crucial; a systematic approach, as detailed in the PALS guidelines, allows for timely intervention. This initial phase informs subsequent steps in the PALS algorithm, guiding decisions regarding oxygenation, ventilation, and potential advanced interventions.
Pediatric Basic Life Support (BLS) Review
A solid foundation in Pediatric Basic Life Support (BLS) is paramount before advancing to PALS, and comprehensive PALS PDF materials reinforce these skills. BLS involves ensuring scene safety, activating emergency services, and initiating high-quality chest compressions at a rate of 100-120 per minute, with a compression depth of approximately one-third of the anterior-posterior diameter of the chest.
Effective ventilation with appropriate bag-valve-mask technique is also critical. The PALS guidelines emphasize minimizing interruptions in compressions and providing adequate oxygenation. Regular review of BLS skills, as detailed in the PALS provider manual, ensures proficiency and readiness for pediatric emergencies.

Managing Pediatric Cardiac Arrest
PALS protocols, detailed in PDF guides, prioritize immediate high-quality CPR, defibrillation when indicated, and prompt vascular access for medication administration.
Asystole and Pulseless Electrical Activity (PEA)
PALS PDF resources emphasize a systematic approach to asystole and PEA in pediatric cardiac arrest. Initiate immediate, high-quality cardiopulmonary resuscitation (CPR), ensuring effective chest compressions and minimizing interruptions. Simultaneously, administer oxygen if the patient is hypoxemic, and promptly attach a monitor/defibrillator to confirm the rhythm.
Continuous monitoring of blood pressure and pulse oximetry is crucial. Establish intravenous (IV) or intraosseous (IO) access as quickly as possible to facilitate medication delivery. While defibrillation isn’t indicated for asystole or PEA, consider advanced airway management and monitor end-tidal carbon dioxide tension (PETCO2) to assess CPR effectiveness. Epinephrine is the primary drug for these rhythms, administered according to PALS guidelines.
Shockable Rhythms: Ventricular Fibrillation (VF) & Pulseless Ventricular Tachycardia (pVT)
PALS PDF guides detail the urgent response to VF and pVT. Immediately initiate CPR while simultaneously preparing for defibrillation. Attach a monitor/defibrillator and deliver the appropriate shock dose based on weight. Continue CPR for two minutes between shockable rhythm checks, minimizing interruptions to chest compressions.
Rapidly obtain IV/IO access to administer medications. Consider advanced airway management and monitor end-tidal CO2 (PETCO2) to guide CPR quality. Epinephrine remains a cornerstone of treatment, administered after unsuccessful defibrillation attempts. PALS protocols emphasize a coordinated team approach for optimal outcomes in these critical scenarios, referencing guidelines updated through 2024.
Airway Management in Pediatric Resuscitation
PALS PDF resources cover advanced techniques like endotracheal intubation, emphasizing careful consideration of pediatric anatomy and appropriate equipment selection for success.
Advanced Airway Techniques
PALS guidelines, detailed within comprehensive PDF manuals, prioritize securing a patent airway in pediatric resuscitation. Advanced techniques extend beyond basic maneuvers, encompassing endotracheal intubation and, less frequently, surgical airway access. Successful intubation requires specialized equipment – appropriately sized laryngoscope blades, endotracheal tubes, and confirmation devices like capnography (PETCO2 monitoring).
The PALS approach stresses preparation and anticipating potential difficulties, given unique pediatric anatomical considerations. Training emphasizes proper tube placement verification, avoiding esophageal intubation. Alternative airway strategies, such as laryngeal mask airways (LMAs), are also addressed as bridging options. Regular review of these techniques, utilizing PALS PDF materials, is crucial for maintaining proficiency and ensuring optimal patient outcomes during critical events.
End-Tracheal Intubation Considerations
PALS PDF resources thoroughly cover end-tracheal intubation, highlighting critical pediatric differences. Accurate age-based equipment selection – blade size, tube diameter – is paramount. Unlike adults, children often require smaller tubes and a more gentle approach. Preoxygenation is vital, alongside careful positioning to optimize visualization of the vocal cords.
Successful intubation demands proficiency in rapid sequence intubation (RSI) principles, including appropriate medication dosages. Post-intubation confirmation, utilizing clinical assessment, auscultation, and capnography (PETCO2), is essential. PALS training emphasizes recognizing and managing potential complications like esophageal intubation or airway trauma. Regular practice and review of PALS guidelines, found in detailed PDFs, are key to mastering this life-saving skill.
Pharmacological Interventions in PALS
PALS PDF guides detail precise drug dosages for pediatric resuscitation, including epinephrine, amiodarone, and lidocaine, based on weight and clinical presentation.
Epinephrine Administration
Epinephrine is a cornerstone drug in PALS, detailed extensively within PALS provider PDF manuals. It’s administered for various conditions, including cardiac arrest, symptomatic bradycardia, and severe anaphylaxis. The recommended dose for cardiac arrest is 0.01 mg/kg (0.1 mL/kg of 1:10,000 solution) via IV/IO, repeating every 3-5 minutes.
For symptomatic bradycardia, the dose is 0.02 mg/kg (0.2 mL/kg of 1:10,000 solution), with a maximum single dose of 1 mg. Careful consideration of vascular access is crucial, favoring IO if IV access is delayed. PALS guidelines emphasize the importance of prompt administration and continuous monitoring during and after epinephrine use, as outlined in current AHA/AAP recommendations from 2020-2024.
Amiodarone and Lidocaine Use
Amiodarone and Lidocaine are antiarrhythmic medications utilized in PALS protocols, comprehensively covered in PALS certification PDF resources. Amiodarone is preferred for shock-refractory ventricular fibrillation/pulseless ventricular tachycardia (VF/pVT), administered at 5 mg/kg IV/IO, potentially repeating once to a maximum of 15 mg/kg.
Lidocaine serves as an alternative if amiodarone isn’t available, dosed at 1 mg/kg IV/IO, repeatable once after 5 minutes, up to a maximum of 3 mg/kg. Careful monitoring for adverse effects, like hypotension, is vital. Current guidelines (2020-2024) emphasize a systematic approach, prioritizing epinephrine before considering these antiarrhythmics, as detailed within the AHA/AAP recommendations.

Post-Cardiac Arrest Care
PALS PDF materials detail post-arrest care, including optimizing ventilation, hemodynamics, and neurological function. Targeted temperature management is also crucial.
Targeted Temperature Management
PALS guidelines, accessible through PDF resources, increasingly emphasize targeted temperature management (TTM) post-cardiac arrest in pediatric patients. This involves maintaining a specific body temperature, typically between 32°C and 36°C, for a defined period – usually 24 hours.
The goal of TTM is to reduce metabolic demand and mitigate secondary brain injury following resuscitation. PDF materials detail the monitoring requirements, cooling and rewarming protocols, and potential complications associated with TTM. Careful consideration must be given to patient-specific factors, and continuous assessment is vital. The 2025 AHA/AAP guidelines continue to refine recommendations based on evolving evidence regarding optimal temperature targets and durations.
Neurological Assessment
PALS PDF guides highlight the critical importance of comprehensive neurological assessment following pediatric cardiac arrest. This extends beyond simply checking for responsiveness and includes evaluating pupillary response, motor function, and brainstem reflexes. Serial assessments are crucial to detect subtle changes and guide further management.
Detailed protocols within PALS materials emphasize the use of validated scoring systems to objectively quantify neurological status. Continuous electroencephalogram (EEG) monitoring may be indicated in select cases to identify seizure activity or assess cerebral function. The 2025 guidelines, informed by recent evidence, reinforce the need for early and ongoing neurological evaluation to optimize patient outcomes and inform prognostication.

PALS and the 2025 AHA/AAP Guidelines
PALS guidelines, often accessed as a PDF, are updated by the AHA/AAP, incorporating recent evidence from 2020-2024 to improve pediatric care.
Key Updates and Changes
PALS guidelines undergo continuous refinement, with the 2025 updates from the AHA and AAP building upon prior revisions from 2020-2024. Accessing the latest PALS PDF is crucial for providers. Recent changes emphasize early epinephrine administration during cardiac arrest, alongside optimized CPR techniques.
The updated guidelines also clarify roles within resuscitation teams, promoting effective communication and coordination. Emphasis is placed on recognizing and addressing the unique physiological differences in pediatric patients. Furthermore, the guidelines incorporate new evidence regarding post-cardiac arrest care, including targeted temperature management and neurological assessment protocols. Staying current with these changes, readily available in the official PALS provider manual and PDF resources, is paramount for delivering optimal care.
Review of Recent Evidence (2020-2024)
A comprehensive review of evidence from 2020 through 2024 significantly informed the 2025 PALS guidelines, readily accessible in the updated PDF format. This included analyses of resuscitation outcomes, pharmacological interventions, and airway management techniques in pediatric populations. Studies highlighted the importance of high-quality CPR and early defibrillation for shockable rhythms.
Research also focused on optimizing epinephrine dosing and the role of alternative vasopressors. The review considered advancements in post-cardiac arrest care, including targeted temperature management and neuroprotective strategies. Accessing the complete evidence summary within the official PALS materials, including the provider manual and downloadable PDF, allows practitioners to understand the rationale behind guideline changes and implement evidence-based practices.

Resources for PALS Learning & Certification
AHA offers comprehensive PALS courses, and a PALS provider manual is available. Convenient PDF versions provide accessible learning and reference materials.
American Heart Association PALS Course
The American Heart Association (AHA) PALS course is the gold standard for healthcare professionals needing to respond to pediatric emergencies. This intensive, classroom-based course blends interactive lectures, simulation scenarios, and skills stations to build confidence and competence. Participants learn to recognize and manage respiratory and cardiovascular emergencies in infants and children, utilizing the latest guidelines.
Course materials often include a detailed PALS Provider Manual, and increasingly, supplemental resources are available in PDF format for convenient study and reference. The AHA continually updates its curriculum based on evolving scientific evidence, ensuring providers are equipped with the most current resuscitation techniques. Successful completion results in a PALS certification card, demonstrating proficiency in pediatric advanced life support principles.
PALS Provider Manual & PDF Availability
The official PALS Provider Manual serves as a crucial companion to the American Heart Association course, offering in-depth coverage of pediatric resuscitation algorithms and pharmacology. It details essential skills, case studies, and current guidelines. While a physical copy is typically included with course registration, digital access is increasingly common.
Many providers seek a PALS PDF version for convenient study on various devices. However, official PDF access is usually restricted to those enrolled in an AHA course, ensuring guideline integrity. Unofficial sources may offer PDFs, but their accuracy and currency cannot be guaranteed. Always prioritize materials directly from the AHA to maintain the highest standard of pediatric advanced life support knowledge.
Pediatric Resuscitation Specific Challenges
PALS addresses unique challenges, like age-related physiology, and differing arrest causes. Mastering these nuances, often detailed in a PALS PDF, is vital.
Age-Related Physiological Differences
Pediatric resuscitation differs significantly from adult care due to substantial physiological variations across developmental stages. Infants and children possess unique characteristics impacting response to illness and injury. A comprehensive PALS PDF resource emphasizes these distinctions, highlighting differences in airway anatomy, respiratory mechanics, and cardiovascular function;
For instance, a smaller airway increases the risk of rapid obstruction, while a larger glottis makes it easier to intubate. Children also have a higher metabolic rate and rely more on oxygen consumption, making them vulnerable to hypoxia. Cardiac output is also dependent on heart rate, not stroke volume, as in adults. Understanding these age-specific nuances, thoroughly explained within PALS materials, is crucial for effective resuscitation and improved patient outcomes. These differences necessitate tailored approaches to airway management, ventilation, and pharmacological interventions.
Unique Pediatric Causes of Arrest
Pediatric cardiac arrest frequently stems from different origins than adult cases, demanding specialized knowledge. Respiratory issues are a primary driver, often linked to asthma, bronchiolitis, or foreign body aspiration. A detailed PALS PDF guide underscores the prevalence of these causes, alongside congenital heart defects and sepsis.
Unlike adults where cardiac events dominate, children often experience arrest secondary to preventable conditions. Trauma, drowning, and sudden infant death syndrome (SIDS) also contribute significantly. Recognizing these unique etiologies is paramount for targeted interventions. The PALS curriculum stresses early identification of underlying causes, emphasizing prompt treatment of respiratory distress and fluid resuscitation for septic shock. Effective resuscitation requires addressing the root problem, not just managing the arrest itself, as detailed in comprehensive training materials.